Premenstrual Dysphoric Disorder
Premenstrual Dysphoric Disorder is a cyclical mood disorder where the brain reacts abnormally to the normal rise and fall of estrogen and progesterone during the luteal phase. Unlike PMS, PMDD is significantly more severe and debilitating — causing intense emotional, cognitive, and physical symptoms that can feel completely overwhelming. You may feel fine one week, then experience suicidal thoughts, rage, or hopelessness the next, only to have everything clear once your period starts.
Abnormal brain sensitivity
People with PMDD don't have abnormal hormone levels — their brains simply react differently to normal fluctuations in estrogen and progesterone. This abnormal sensitivity triggers severe mood symptoms that feel utterly disproportionate to anything happening in your life.Frequently misdiagnosed
PMDD affects approximately 1 in 20 women, but it's often mistaken for anxiety, depression, or 'just PMS.' Many suffer for years before receiving an accurate diagnosis. The cyclical pattern — symptoms appearing during the luteal phase and resolving with menstruation — is the key distinguishing feature.Treatment options available
Treatment may include SSRIs (often effective at lower doses than for depression), hormonal therapies, and lifestyle modifications. Emerging brain-based approaches target the nervous system's heightened sensitivity to hormonal fluctuations, offering new hope for those who haven't found relief with traditional treatments.Possible Causes of Premenstrual Dysphoric Disorder
Abnormal hormone sensitivity
People with PMDD don't have abnormal hormone levels; their brains simply react differently to normal fluctuations in estrogen and progesterone. During the luteal phase, when these hormones rise and then drop, the brain's response triggers severe mood symptoms.
Serotonin dysfunction
Hormonal changes affect serotonin, a neurotransmitter that regulates mood, sleep, and appetite. In PMDD, the luteal phase hormonal shifts appear to disrupt serotonin activity more severely than in people without the condition.
GABA system changes
GABA is a neurotransmitter that promotes calm and relaxation. Progesterone metabolites normally enhance GABA activity, but in PMDD this system appears to function abnormally, potentially contributing to anxiety and mood symptoms.
Genetic factors
PMDD tends to run in families, suggesting genetic vulnerability. Recent research has identified specific gene variations affecting how cells respond to estrogen and progesterone.
Inflammatory response
Some research suggests that PMDD may involve an abnormal inflammatory response to hormonal changes, affecting brain function and mood regulation.
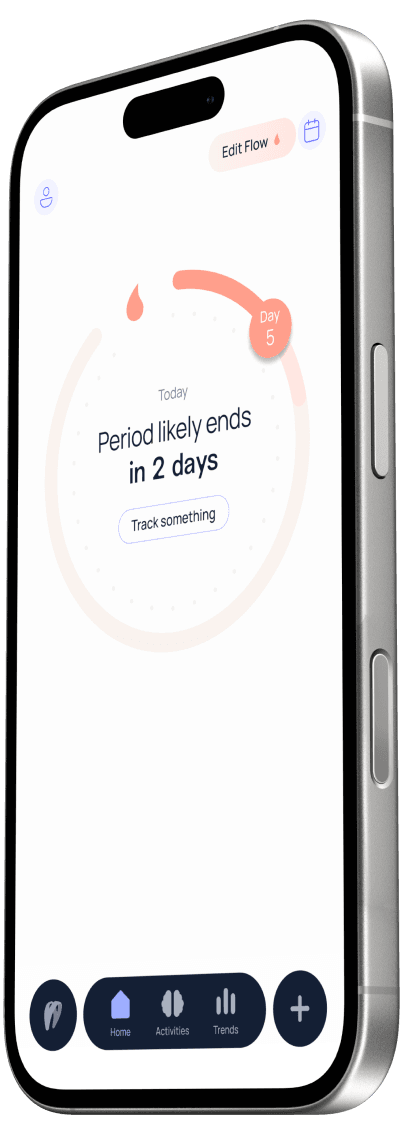
Your experiences with precision
The Samphire App helps you track a comprehensive range of symptoms, giving you the insights you need to better understand your experiences and communicate effectively with those around you.
Severe mood swings
Sudden sadness, tearfulness, or emotional sensitivity that feels disproportionate to your circumstances
Feeling out of control
Feeling unable to cope with normal responsibilities or like a different person during your luteal phase
Intense irritability or anger
Feeling rage or having increased interpersonal conflicts that are out of character
Sleep changes
Insomnia or hypersomnia — difficulty falling asleep, staying asleep, or sleeping excessively
Depressed mood or hopelessness
Feelings of worthlessness, despair, or suicidal thoughts during the luteal phase
Breast tenderness
Soreness, swelling, or painful sensitivity in the breasts
Severe anxiety or tension
Feeling on edge, panicked, or overwhelmed by normal responsibilities
Joint or muscle pain
Generalized aches and pains, often in the lower back, joints, and limbs
Difficulty concentrating
Brain fog that makes it hard to focus on work, conversations, or daily tasks
Bloating or weight gain
Fluid retention and abdominal swelling during the luteal phase
Loss of interest in activities
Withdrawal from activities you normally enjoy, feeling disconnected or numb
Headaches
Tension headaches or migraines triggered by hormonal fluctuations
Treatment Landscape
The Options Available
PMDD treatment typically combines multiple approaches. What works varies individually, and finding the right combination often requires patience and medical support.
SSRIs (antidepressants)
First-line treatment for PMDD. Can be taken daily or only during the luteal phase, and are often effective at lower doses than those used for depression.
Hormonal birth control
Birth control pills (particularly those with drospirenone) help stabilize hormonal fluctuations. Continuous contraception can eliminate periods entirely.
GnRH agonists
Suppress ovulation to eliminate hormonal cycling in severe cases. Creates a temporary menopause-like state.
Anti-anxiety medications
For acute symptom management during the most challenging days of your cycle.
Surgical options
Hysterectomy with removal of ovaries — only considered for severe, treatment-resistant cases after all other options have been exhausted.
Non-invasive neurostimulation
Brain-based approaches that support emotional regulation and reduce the nervous system's reactivity to hormonal shifts.
Cognitive behavioral therapy
CBT specifically tailored for PMDD, helping to build coping strategies and manage the emotional impact of cyclical symptoms.
Mindfulness and movement
Mindfulness-based interventions, gentle yoga, and regular exercise help regulate the nervous system and reduce symptom severity.

Brain-based relief
Lutea™ supports overall wellbeing across your cycle through gentle neurostimulation — no hormones, no drugs, no known interactions.

Brain-based relief
Lutea™ supports overall wellbeing across your cycle through gentle neurostimulation — no hormones, no drugs, no known interactions.
Our Blog
Selected articles
Dos and Don'ts
Most Common Questions
Here are some of the most common questions about premenstrual dysphoric disorder we receive from our community.
We see patterns others ignore.
Too often, systems treat symptoms in isolation. Our solutions work across the brain, body and cycle - connecting the dots between pain, mood, focus, hormones and more.
For educational purposes only
This information should not replace professional medical advice. Always consult with your healthcare provider for personalized medical guidance.
Contact Support